A diagnosis of prostate cancer is alarming. But its progression can be so slow that many live out their normal life spans without experiencing problems. The average age of onset for prostate cancer is 66, but about 80 percent of men who reach age 80 live with cancer cells in their prostate.
What is active surveillance?
With active surveillance, treatment isn’t the first course of action when prostate cancer is diagnosed. Rather, tests and exams are scheduled at regular intervals to monitor for changes. If the cancer doesn’t change and remains in the low-risk category, the tests continue about every six months. If the cancer grows or other changes cause concern, a doctor may recommend surgery or other more invasive actions. Active surveillance is most appropriate for early stage cancer found in only one area of the prostate gland, and the patient displays no symptoms. The point is to avoid the side effects that more aggressive treatments can cause, such as impotence and loss of bladder control. About 92 percent of all prostate cancers are found in the early stage.
Who should be screened and at what age?
While all men are at risk of prostate cancer, African-Americans and those with a family history of prostate cancer face a higher risk and may want to begin screening as young as age 40. Health organizations offer differing guidelines, but the U.S. Preventive Services Task Force recommends that all men age 55 and up to age 69 talk with their doctor about the pros and cons of screening for prostate cancer.
About prostate cancer and screening
Prostate cancer is the second most common cancer among men in the United States. It can also be a very slow-growing cancer, so it makes sense not to rush into treatment and invite the potential side effects associated with surgery, radiation, and drugs. A Johns Hopkins study of men with low-risk prostate cancer found that after 15 years of active surveillance, less than one percent of them experienced a spread of the disease, called metastasizing.
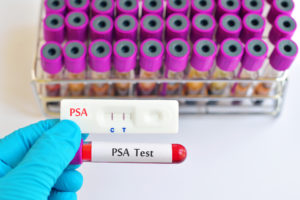
Screening for prostate cancer is done via a prostate specific antigen (PSA) blood test that measures protein levels in the prostate gland. A high PSA count (4 or above) may be an indication of prostate cancer, but it can also be a marker of non-cancerous conditions such as an enlarged prostate or infection. Experts say there’s really no “normal” PSA number, but generally, the lower the number, the less you have to worry about prostate cancer.
An elevated PSA count can result from symptom-free tumors that are unlikely to present a risk to a man’s life. This is a serious downside of screening called overdiagnosis, and its effects are not inconsequential. The National Cancer Institute reports that only about 25 percent of the men undergoing a biopsy because of an elevated PSA count actually had cancer.
Additional tests help determine appropriate action
If your PSA count is high, your doctor may order an M.R.I. and biopsy to hone in on whether prostate cancer is indeed present. The M.R.I. can reveal suspicious lesions. A biopsy allows a pathologist to compare sample prostate tissue with normal tissue and gauge how aggressive the cancer may be. The pathologist looks for the specific area or areas where cancer may be lurking, and the volume of cancer cells. Advances in technology currently under study may bring about less invasive procedures, such as urine and biomarker tests, providing a less expensive and reliable alternative to current M.R.I. and biopsy procedures.
After analysis, the biopsy results are compiled into a Gleason score. As with the PSA count, a lower Gleason score indicates a lower risk. Someone with a Gleason score of 6 or lower, coupled with a PSA count of 4 or lower would be a good candidate for active surveillance. In fact cancer experts have debated over the years whether a Gleason score of 6 or less should even be labeled as cancer.
The National Cancer Institute reports that only about 25 percent of the men undergoing a biopsy because of an elevated PSA count actually had cancer.
Risks v. benefits of active surveillance
After reviewing test results and physical examination, your doctor will offer an opinion about the best course of action. In addition to test scores, other factors should be taken into account when deciding whether active surveillance is appropriate. Getting a second opinion, particularly from a healthcare facility designated as a center of excellence for prostate cancer care, can assure you’re getting access to highly skilled experts at the forefront of their field.
- Younger men with a less aggressive prostate cancer may want to hold off on procedures that effect their erectile and urinary function.
- Men who have other serious diseases such as heart disease, high blood pressure or diabetes may have concerns that these conditions could worsen with invasive prostate cancer surgery or radiation.
- The anxiety of knowing that prostate cancer is present and not knowing for certain how quickly it may progress, makes some men uneasy with waiting to remove it, and they may prefer full surgical removal. Prostate focal therapy is a less invasive procedure whereby a single area of the prostate containing a small amount of cancer is removed. There is a lower risk of side effects with focal therapy, but also a risk that not all of the cancer will be removed. If prostate focal therapy is selected, active surveillance after the procedure would be prudent.
- Full surgical removal and treatment with radiation and drugs may be pursued if the cancer is growing quickly and/or spreading to other areas. This may be the initial recommendation or after active surveillance indicates a change for the worse.
What is watchful waiting?
Active surveillance is most appropriate for men having the time to wait – sometimes decades – before surgical or other advanced procedures are necessary. If life expectancy, due to physical condition or age, is fewer than 10 years, a more useful approach known as watchful waiting may be a better option. Watchful waiting bypasses the battery of testing associated with active surveillance, and instead focuses on responding to symptoms such as extreme fatigue or urinary retention that affect quality of life. Avoiding the possibility of pain, hassles, and complications from continual biopsies, exams, and other procedures makes sense if surgery is not a viable option.
Great survival rates for early stage prostate cancer
Prostate cancer awareness is important, especially given the prevalence with which it occurs. About 1 in 7 men are diagnosed with it in their lifetimes. Thankfully, it’s frequently slow growing and spreading. As a result, almost 100 percent of men found to have early stage prostate cancer survive more than five years after diagnosis. The American Society of Clinical Oncology indicates a 15-year survival rate in 96 percent of cases.



